
Children with Diabetes
Type 1 diabetes is the most widespread form of diabetes in children and adolescents. Currently, about 30,000 to 32,000 minors in Germany have diabetes. About 2300 new cases are diagnosed every year. According to various forecasts, the number of people with diabetes will increase in the coming years. Since the insulin-producing cells of diabetes patients are destroyed by their own immune system, they have to supply themselves with the hormone.

Children and diabetes.

Children and overweight.
However, it is becoming increasingly common for children and adolescents to also develop type 2 diabetes. As a rule, this form of diabetes only appears after the age of 40. Since children increasingly eat insufficiently and suffer from obesity and lack of exercise, type 2 diabetes is also becoming more common in young people. About 200 children between the ages of 12 and 19 are estimated to develop type 2 diabetes.
There are even rarer cases of diabetes in adolescence. These include MODY (Maturity-Onset Diabetes in the Young). There are currently no reliable estimates of the number of children and adults with the disease.
Symptoms of diabetes in children
Only when about 80 percent of the insulin-producing beta cells in the child’s pancreas have been destroyed do the first symptoms usually appear. Before this event occurs, the remaining amount of insulin is sufficient to avoid a complete derailment of the sugar metabolism.

Diabetes and nutrition in children.
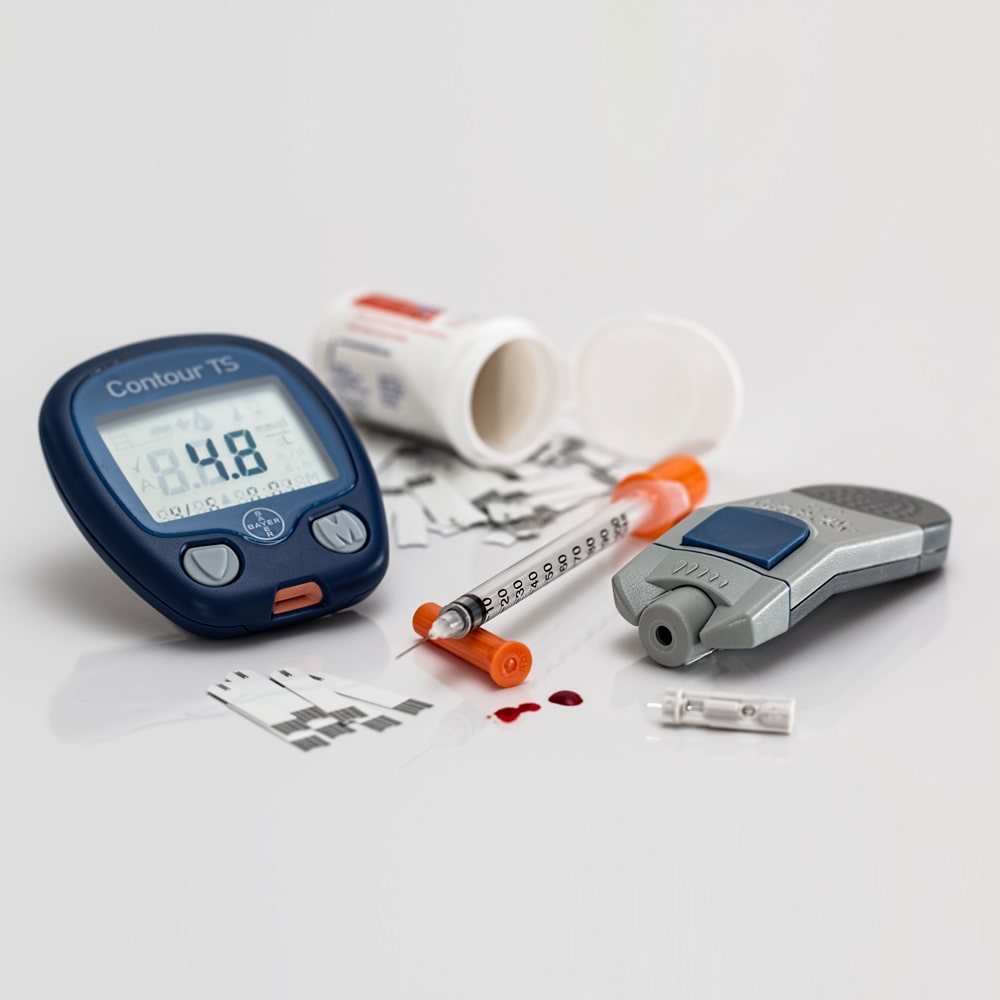
Diabetes meter, insulin syringe and tablets.
Symptoms of children with type 1 diabetes include:
- Frequent and nocturnal urination up to and including enuresis.
- Intense feeling of thirst and the associated large amount to drink
- Weakness in performance and general tiredness
- Weight loss despite permanent ravenous appetite (underage diabetes type 1 patients are usually slim)
- Intense abdominal pain
- In advanced stages, exhaled air may have a typical acetone odour (similar to that of nail polish remover)
Symptoms develop more slowly in children with type 2 diabetes. Although they are similar to those of type 1, children with type 2 diabetes often suffer from severe obesity.
Risk factors and causes of children with diabetes
Both the causes and the risk factors depend on the type of diabetes.
Type 1 diabetes in children and teenagers
Type 1 diabetes is an autoimmune disease. The insulin-producing beta cells in the pancreas are attacked by antibodies and destroyed. This results in a lack of insulin.
Many of these autoantibodies of diabetes type 1 are now known. These include, for example, autoantibodies against insulin (IAA) and cytoplasmic islet cell components (ICA).
It is still unclear why the immune system attacks its own tissue. Since type 1 diabetics often have other diabetics in the family, genetic factors, among others, seem to play a role. In the meantime, research teams have identified various gene mutations that suggest a connection with type 1 diabetes.
In addition, certain infections seem to be involved in the development of diabetes. These include measles, rubella and mumps. Researchers are also currently discussing whether breastfeeding for too short a period of time could be the cause of diabetes or whether gluten-containing foods and cow’s milk are given prematurely.
Did you know that type 1 diabetes often occurs in combination with other autoimmune diseases such as Addison’s disease or coeliac disease?
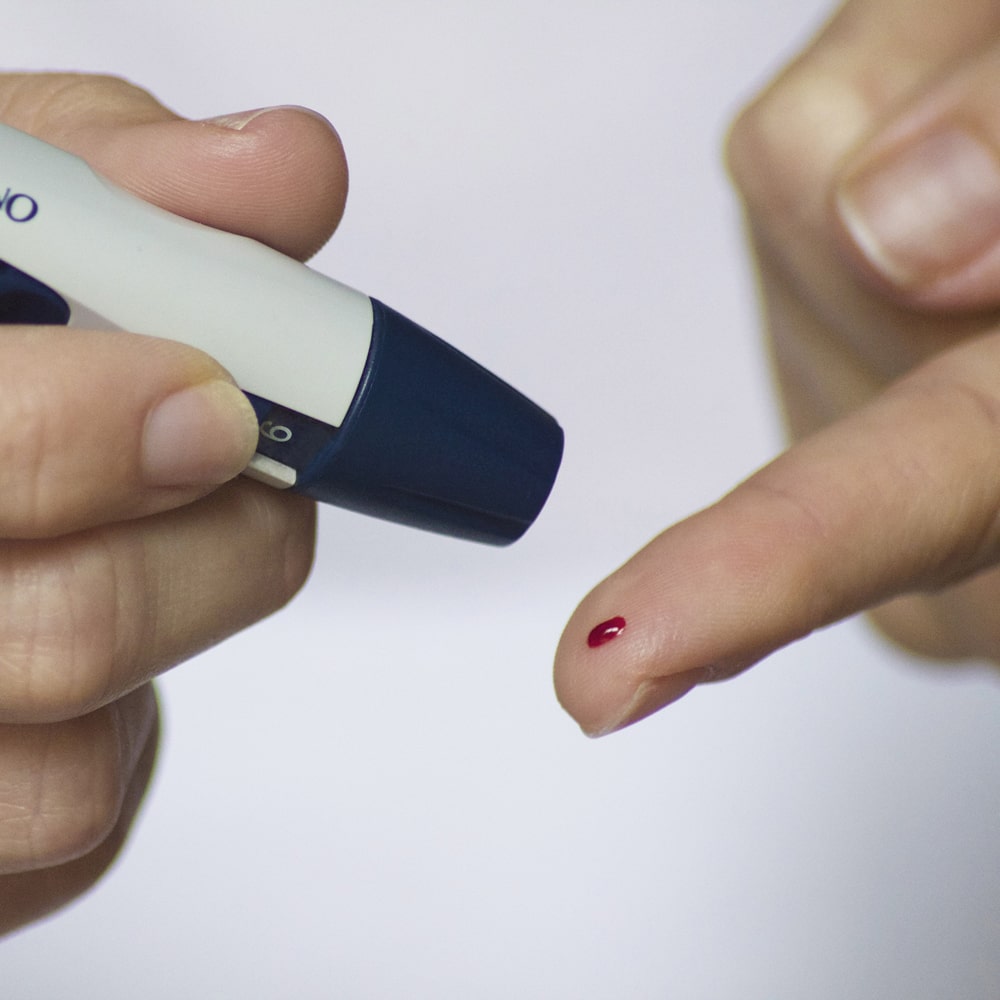
Finger and Diabetes measuring Blood Glucose.

Scale and blood glucose measurement.
Type 2 diabetes in children and adolescents
Unlike type 1, type 2 diabetes develops over years. Over time, the body’s cells begin to react less and less sensitively to the hormone insulin. Eventually, a relative insulin deficiency occurs. The amount of insulin produced by the pancreas is still sufficient, but its effectiveness decreases. For this reason, the pancreas begins to produce more and more insulin. This leads to an overload of the organ and eventually to complete exhaustion. In many cases, an absolute insulin deficiency develops.
Concrete causes of type 2 diabetes are still unknown to scientists. However, there are a number of risk factors that favour insulin resistance. These include, for example, lack of exercise or an unhealthy diet. These risk factors apply equally to children and adults.
Special forms of diabetes in minors
Special forms of diabetes, which usually only occur in adults, can in rare cases already break out in childhood. These early diseases are called MODY (Maturity Onset Diabetes of the Young). These diseases are caused by genetic defects in the insulin-producing cells in the pancreas. The term MODY is also known by scientists and doctors as diabetes type 3a.
There are other numerous forms of diabetes, all with different causes (e.g. drugs, viruses or chemicals).

Diabetes Insulin Hyperglycemia

Obesity and the scale.
Common diabetes myths
There are a lot of rumours and falsehoods about diabetes. Which are true and which are not? You can read about this and more here with us:
Every diabetic has to inject themselves with insulin.
Not true. Only people with type 1 diabetes need to inject insulin. To keep blood sugar levels under control, it is usually enough for type 2 diabetics to pay attention to their diet and overall lifestyle. For them, insulin therapy is the last alternative.
Everyone who eats a lot of sweets automatically gets sick.
This is not entirely true either. However, people who eat an excessive amount of chocolate, jelly babies or other sweets gain weight more easily. Being overweight is more likely to lead to type 2 diabetes, whereas eating sweets is not a risk factor for type 1 diabetes.
Young people are not affected by adult-onset diabetes.
Even though the name adult-onset diabetes comes from an increased risk of getting the disease in old age, minors are also getting type 2 diabetes more and more often.
Small excess amounts of sugar are not harmful to the blood.
The most important thing is how long the blood is exposed to the high amount of sugar. If the sugar level in the blood is elevated for too long, it can damage the blood vessels. This, in turn, can lead to a heart attack or stroke in the worst case.
Every diabetic is overweight.
Most people with type 2 diabetes are actually overweight. However, patients with other forms of diabetes, such as type 1 diabetes, are usually of normal weight.
Insulin therapy must be given for life.
For patients with type 1 diabetes, this is true. Type 2 diabetics may be lucky that insulin therapy is only needed for a while. However, the metabolic condition can often be improved with a change in diet or weight loss.

Overweight Tape Measure Diet.

Diabetes and nutrition.
A specific diet is compulsory
This used to be the case. Nowadays, however, diabetics are recommended to eat the same balanced diet as healthy people. This includes fruit and vegetables as well as carbohydrates, fibre, animal proteins and little sugar. For diabetics, however, it is important to pay attention to the amount of carbohydrates.
Products specifically for diabetics make sense.
This is nonsense. Diabetics do not need special foods. These can even be counterproductive. Especially if they contain a lot of fat and thus calories. Moreover, these diabetic products are often completely overpriced.
Sugar is absolutely forbidden for diabetics.
If their blood sugar is well controlled, diabetics can very well consume sugar, although only in a very limited way. As an alternative, diabetics can use sweeteners such as aspartame, Stevia or acesulfame. They are all virtually calorie-free and do not affect blood sugar levels.
Diabetes mellitus lasts a lifetime.
It is true that type 1 diabetes cannot be cured. In principle, this is also true for type 2 diabetes, but with consistent therapy and extensive lifestyle changes, the metabolic situation can at least stabilise to such an extent that the patient hardly experiences any symptoms in everyday life. The only form of diabetes that usually disappears is gestational diabetes.
Examinations and diagnosis in children with diabetes
If diabetes is suspected in your child, a paediatrician or internal medicine and endocrinology specialist is the right person to contact. They will most likely be asked the following questions:
- Has your child often been noticeably tired lately?
- Does he or she have to urinate frequently or wet himself or herself at night?
- Has he or she been drinking more lately or complaining of thirst?
- Does he or she complain of stomach aches?
- Have you noticed a fruity smell (like “nail polish remover”) on their breath?
- Does another family member have diabetes?

Diabetes and a balanced diet | Fruit and vegetables.
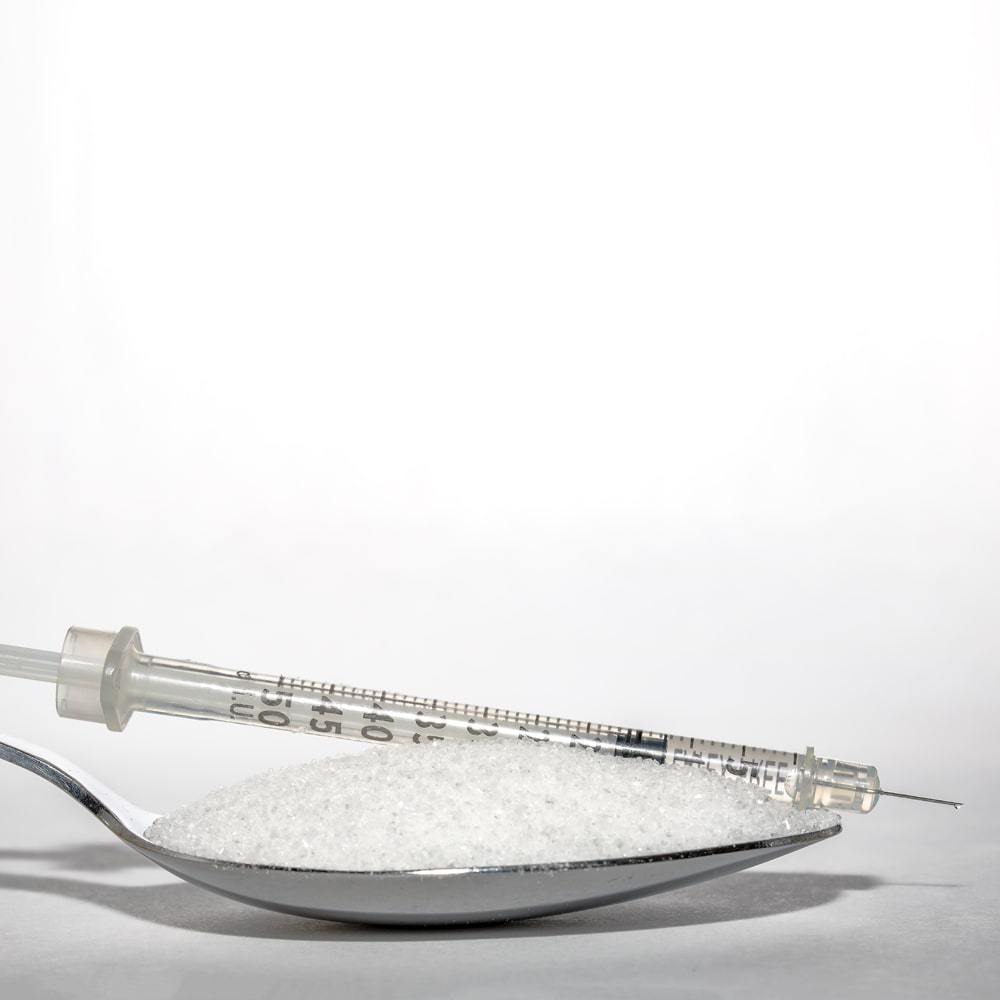
Diabetes Spoon Sugar and Insulin Syringe.
Physical examination and fasting blood glucose level
After the doctor has examined your child, a new appointment is usually made for the morning blood sample. It is especially important that your child comes to the blood test fasting, i.e., that he or she has not eaten anything eight hours beforehand. Otherwise, a reliable result of the fasting blood glucose value cannot be guaranteed. A single blood sugar measurement is not sufficient for a diagnosis. Repeated measurements ensure that measurement errors and fluctuations can be excluded. If all results are above 126 milligrams per decilitre of blood, diabetes mellitus is likely.
The long-term blood glucose value (HbA1c)
The long-term blood glucose value indicates the average blood glucose level over the last two to three months. If the blood glucose level is repeatedly too high or remains too high for a long time, “sugared” haemoglobin is formed. Circulating sugar molecules attach themselves to the red blood pigment. The exact proportion of total haemoglobin is determined in the laboratory and given as a percentage. Diabetes is very likely to be present if the value is more than 6.5 percent.
However, the HbA1c method is usually only carried out in children and adolescents in cases of doubt.
In order to be able to determine the success of a diabetes therapy, the HbA1c value is also carried out if the diagnosis is already known.
The antibody screening test
In the case of an ambiguous type 1 diagnosis, a so-called antibody screening test can bring clarity. To do this, the patient’s blood is tested for antibodies typical of type 1 diabetes. This antibody test is not possible for type 2 diabetes.
An antibody screening test offers the advantage that a diagnosis of diabetes type 1 in minors is possible very early. It is possible to detect autoantibodies in the blood years before the onset of the disease. This is because by the time the symptoms appear, 80 percent of the beta cells in the pancreas have already been destroyed.
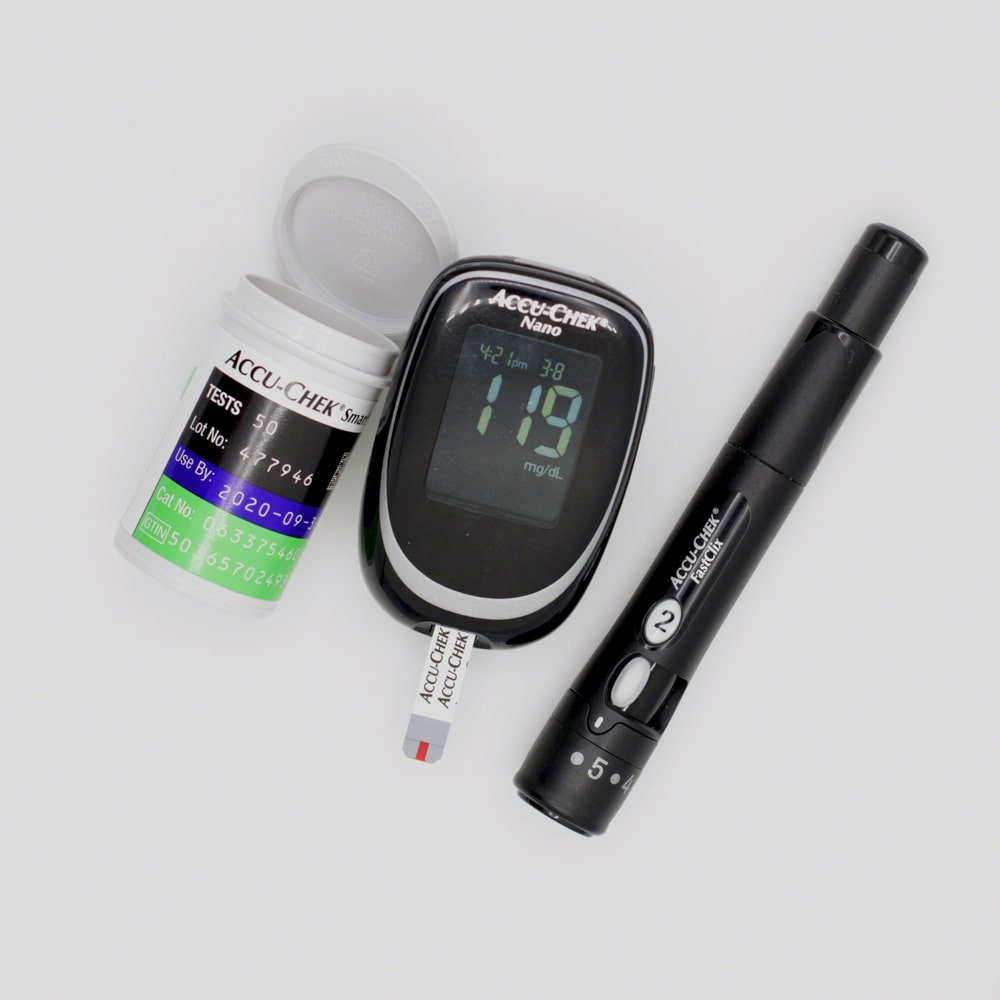
Diabetes Test Strips and Blood Glucose Tester.

Regularly check cardiovascular health with diabetes.
The oral glucose tolerance test (OGTT)
The oral glucose tolerance test or sugar load test checks how well or poorly the body can process sugar. The first step is to determine the fasting blood glucose level. Next, the patient must consume a specific sugar solution (75 grams of dissolved sugar). The blood sugar is then measured both after one and two hours. If the values exceed set limits, there are many indications that the patient has diabetes.
The OGTT is also usually only carried out in cases of doubt in minors. If diabetes type 2 is suspected, however, the test is part of routine diagnostics. To avoid mistakes, it is often carried out twice.
Examination of the urine
In order to make a definite diagnosis, doctors often also do a urine test for glucose. Under normal circumstances, the sugar that enters the primary urine is transported back into the bloodstream by certain cells in the kidney marrow. So, no sugar should be detectable in the blood of a healthy person. However, if the blood sugar level is too high, the kidney may no longer be able to reabsorb it. In this case, the sugar is excreted in the urine. This can be an indication of glucose intolerance or diabetes.
In the meantime, there is also a test strip that can be used to detect glucosuria from home. The result can be read within a few minutes.
If the blood sugar level is permanently too high, the kidney tissue can be damaged by the sugar molecules. This is called diabetic nephropathy. The so-called albumin is a protein in the urine and an indication of diabetic nephropathy. This can also be detected with a urine test strip.
Further examinations
Further examinations are necessary as soon as diabetes type 2 has been diagnosed in minors. This is to detect possible concomitant diseases. These concomitant diseases include, for example, lipometabolic disorders, diabetes-related eye diseases or high blood pressure. In most cases, such secondary diseases are already present at the time of diagnosis.
Treatment of underage diabetes patients
Special diabetes training courses are offered for parents as well as for the children themselves, which can be very helpful immediately after the diagnosis. The content is mainly about the disease itself (development, course) and the various treatment options. The amount of carbohydrates in various foods, the hormone insulin and possible complications (hypoglycaemia or hyperglycaemia) are also explained.
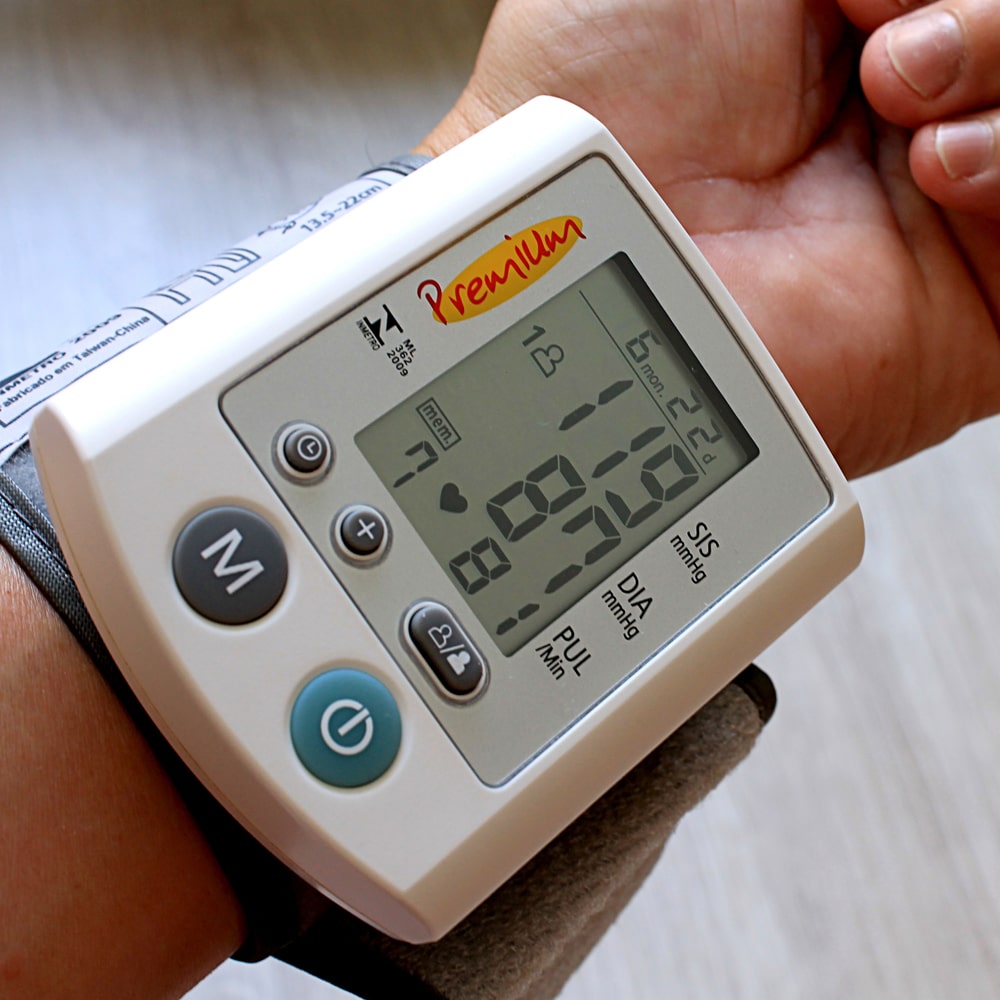
Blood pressure monitor | Measure blood pressure.
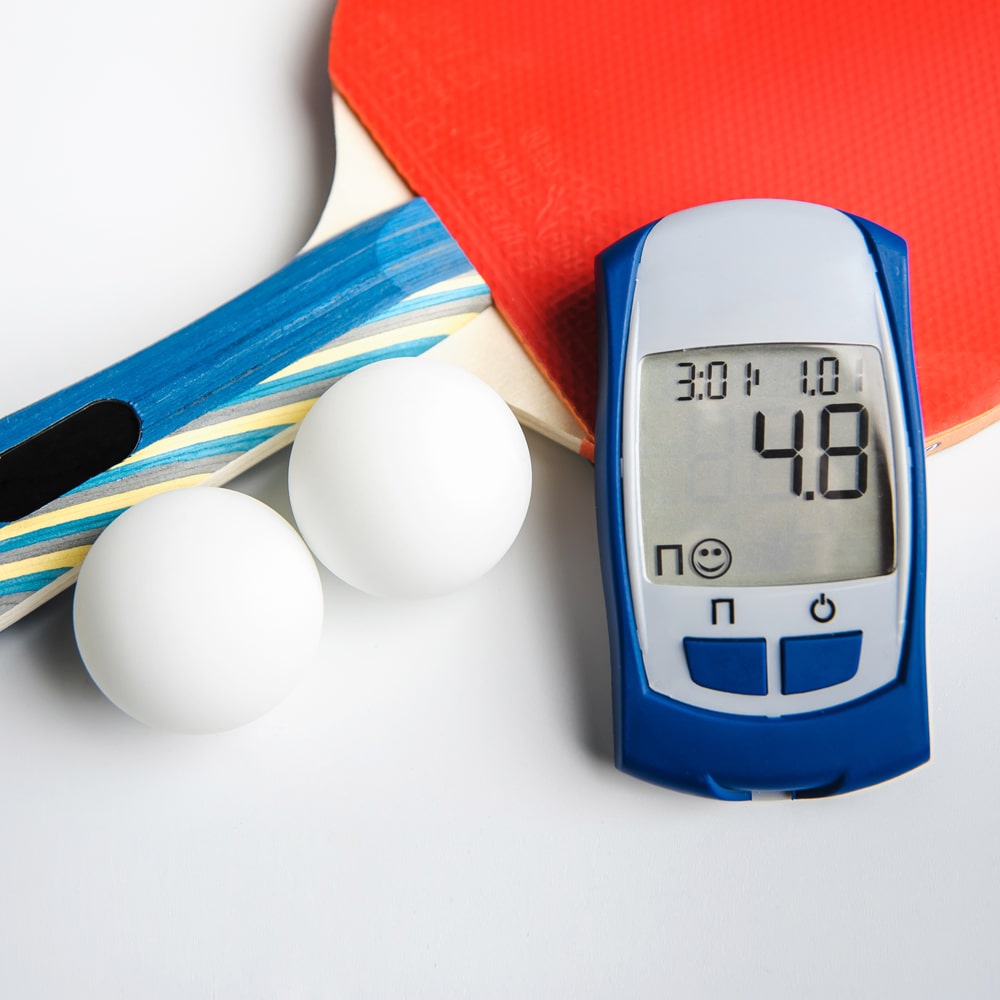
Diabetes Blood Glucose Test Device and Sports Exercise.
Treatment of underage type 1 patients
The body of a type 1 patient is dependent on the injection of insulin for life. The pancreas is no longer able to produce the hormone itself. Nowadays, insulin is usually administered as part of intensified insulin therapies or with the help of insulin pumps. This can be controlled particularly quickly and, above all, flexibly.
In training, type 1 diabetes children learn at what time the body needs which amount of insulin. This is essential, as otherwise life-threatening hypoglycaemia or hyperglycaemia can occur. The children are also taught how to use the insulin syringes correctly.
Therapy goals as well as the type of diabetes therapy are determined individually for each patient. An example of this is the HbA1c therapy. Here, values below 7.5 percent are usually preferred.
Intensified insulin therapy (basic bolus principle)
This therapy model involves injecting insulin once or twice a day. This is to balance the basic insulin requirement (baseline). Diabetes patients have to measure their blood sugar level before each meal and then inject themselves with normal or short-acting insulin (bolus). The required bolus amount depends on the time of day as well as the composition of the respective meal.
The insulin pump
In order to keep the quality of life as high as possible despite the disease, insulin pumps are often used, especially in children. For this purpose, a thin needle is implanted in the abdominal fat and connected to a battery-operated insulin pump via a small tube. The small, programmable pump is equipped with an insulin reservoir and can be attached to a belt, for example.
Distributed throughout the day, the insulin pump releases defined amounts of insulin into the body’s fatty tissue. From here, the hormone reaches the rest of the body through small blood vessels. At the touch of a button, the patient can administer additional amounts at meals.
The insulin pump gives those affected a lot of freedom. It also takes a lot of pressure off children with diabetes, because the daily painful insulin injections are no longer necessary. The insulin pump can always be worn, even during sports or play. However, if necessary – for example, for swimming – the pump can also be disconnected for a short time.
The insulin pump is individually adjusted in a specialised diabetes practice or clinic. The insulin reservoir (cartridge) is replaced or refilled regularly.
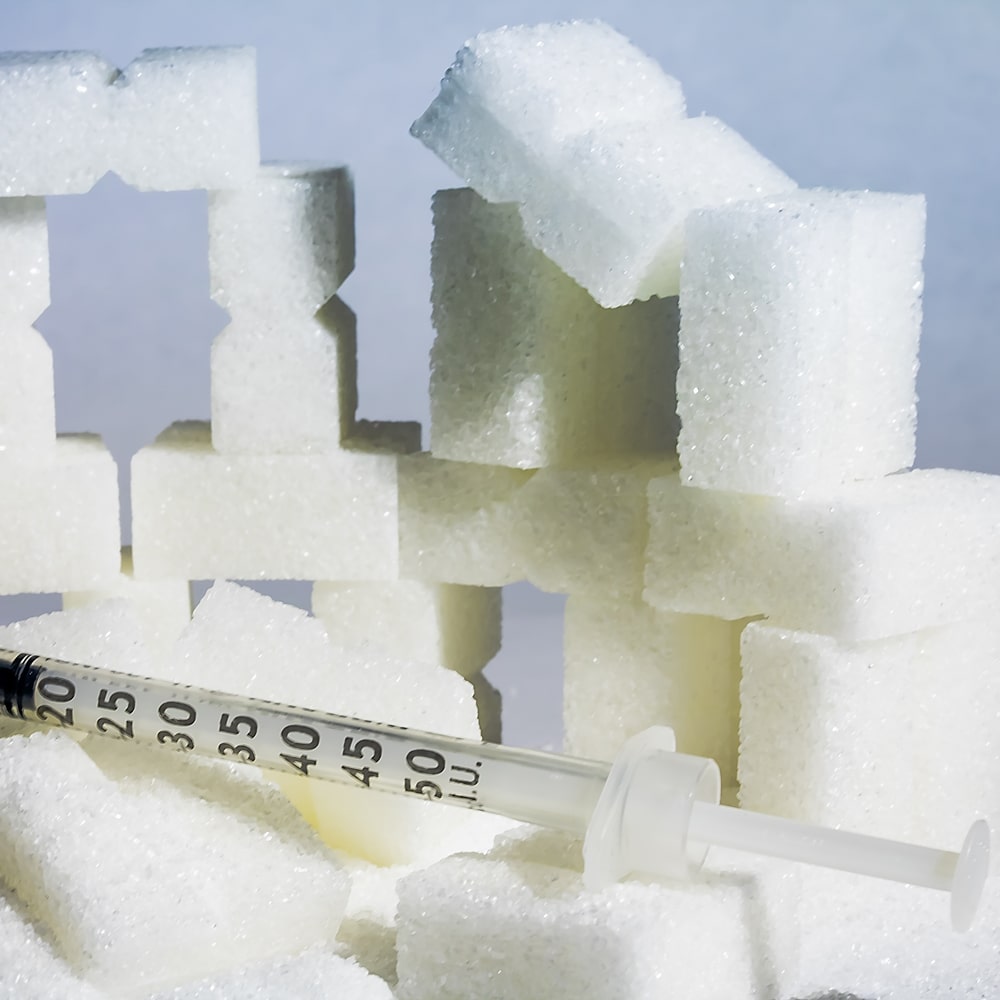
Diabetes Sugar and Insulin Injection.

Overweight Tape Measure Diet.
The treatment of type 2 diabetes in children
An individual therapy plan and therapy goals are set as for type 1 diabetes.
Regular physical activity, sport and a change in diet form the basis of the treatment. The diet should be rich in fibre and include plenty of fruit and vegetables. It reduces the risk factors for concomitant or secondary diseases, especially high blood pressure and cardiovascular diseases. It also helps diabetes patients to reduce their weight and lower their blood sugar.
Diabetes children receive tips and help, individual dietary advice and an exercise programme in diabetes training courses.
There are type 2 diabetes patients who can get their diabetes under control through more physical exercise, weight loss and a diabetes diet. However, the tendency to diabetes persists and therefore blood glucose levels need to be checked regularly.
If it is not possible to motivate young diabetes patients to change their lifestyle by changing their diet and increasing their physical activity in order to lower their blood sugar, the doctor will prescribe diabetes medication (antidiabetics). This is usually attempted with metformin tablets, an oral antidiabetic. If the therapy is not successful, the diabetes patient is given insulin after about 3-6 months.
Treatment of concomitant and secondary diseases of diabetes
Course of the disease and prognosis in children with diabetes.
In children and adolescents with type 2 diabetes, a change in lifestyle is decisive for the course of the disease. In some cases, it can disappear completely through an adapted diet, weight loss and more exercise and sport.
Type 1 diabetes is still incurable. It affects children, adolescents and adults. Regular medical check-ups and training are indispensable. To avoid secondary diseases, it is necessary to achieve constant blood sugar levels through insulin therapy. As a general rule, the risk of secondary damage is higher in young diabetes patients.
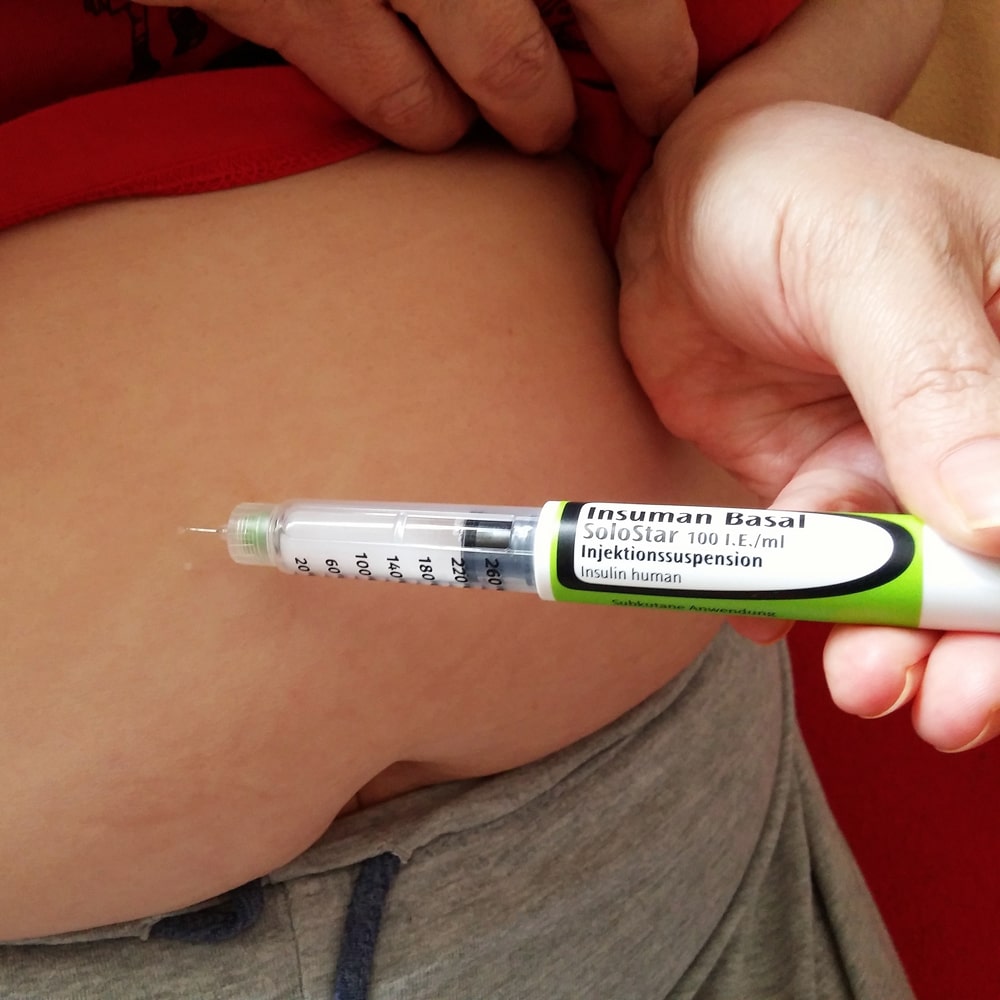
Insulin injection.

Diabetes | Regular exercise is important for a healthy lifestyle.
The main goal is to achieve blood glucose levels that are as constant as possible in order to avoid secondary diseases. In principle, the younger the age of the patient, the higher the risk of secondary diseases later in life.
Acute complications can occur with varying frequency in both type 1 and type 2 diabetes. These are primarily hypoglycaemia and hyperglycaemia. Especially in type 1 diabetes, hyperglycaemia can lead to diabetic ketoacidosis in severe cases.
Hypoglycaemia | Low blood sugar
In children on insulin therapy, one of the most common and dangerous acute complications is hypoglycaemia. This often occurs when heavy physical exertion results in too much exercise or when too much insulin has been injected by mistake. In type 2 diabetes, an overdose of blood sugar-lowering tablets or skipping meals can also be other causes.
A pronounced feeling of weakness, palpitations, dizziness, sweating and trembling hands can be possible symptoms of hypoglycaemia. Concentration and vision disorders, impaired consciousness, unconsciousness and convulsions can occur in severe cases.
It is recommended that diabetics who have to take insulin always have glucose with them. This helps the blood sugar to rise quickly in case of a slight hypoglycaemia. Medical treatment is usually necessary in severe cases.

Regular drinking with diabetes.

A healthy diet is important for diabetes.
Diabetic ketoacidosis
In type 1 diabetes children, the absolute lack of insulin means that sugar (glucose) can no longer be absorbed from the blood into the cells. The blood sugar continues to rise if the body is given no insulin at all or too little. In acute infections such as a urinary tract infection or pneumonia, such hyperglycaemia occurs in insulin-dependent diabetics. Even if the patient eats little, the body then needs more insulin than normal. As a result, the blood sugar rises excessively because the normal insulin dose is not sufficient.
There is a glucose deficiency in the cells and thus a lack of energy when there is excess glucose in the blood, because there is a disproportionate amount of glucose there. The brain, which depends on glucose for energy, needs a particularly large amount of energy. The body begins to break down more fat to compensate for the energy deficit. This produces ketone bodies, which leads to acidification of the blood, which is called diabetic ketoacidosis.
Very deep breathing, the fruity acetone smell of the exhaled air are typical symptoms. The body tries to reduce the high blood sugar level by excreting sugar together with a lot of fluid.
The result is increased urine output, which leads to dehydration. In extreme cases, patients can fall into a comatose state (ketoacidotic coma) as they become tired and weak. In such a situation, the emergency doctor (telephone: 112) must be called immediately, as the coma means danger to life, and the patient must receive intensive medical treatment.
Note:
Your Content Goes Here
Consequential diseases in diabetes
Diabetic foot syndrome can be caused and triggered by nerve damage combined with vascular damage due to high blood sugar. The nerve damage, along with vascular damage that also becomes, can trigger diabetic foot syndrome.
Possible late effects can occur in untreated or poorly controlled diabetes, not only in children and adolescents but also in adults. These possible late effects are in particular heart attacks and strokes.